We all have medical questions that we want answered – that’s why Dr. Amna Asif is here to provide us with her expert opinion! Every other week, she will be sharing her expert advice with us regarding a range of topics our followers are interested in learning more about. This week in Doc Talk, she talks about osteoarthritis. Read ahead to find out what exactly it is, what the causes and symptoms are, and what you can do to treat it:
What Is Osteoarhritis?
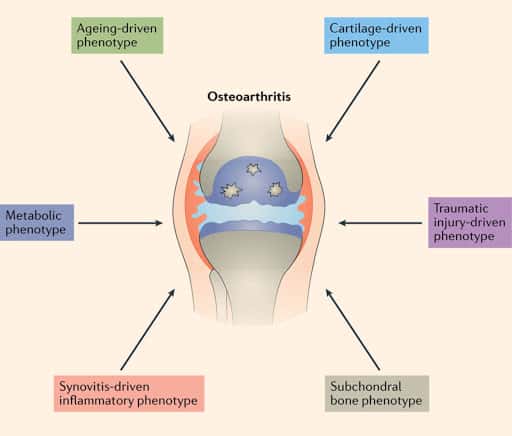
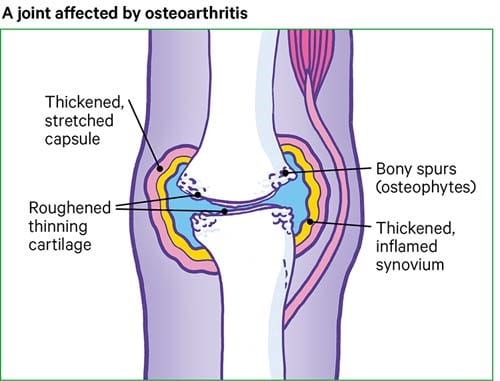
Osteoarthritis is a chronic condition where the joints in your body become inflamed and damaged. Over time, the bones in the joints rub together, causing pain, stiffness, swelling and reduced movement. This can make it harder to walk, climb stairs or do other daily activities. It can worsen overtime, though Osteoarthritis is not an inevitable consequence of ageing and can be managed effectively.
This condition can affect any joint in the body, but mostly affects knees, hips, finger joints and feet.
Prevalence
Osteoarthritis is a common type of Arthritis in Pakistan. Women are more likely to develop osteoarthritis than men; about 1 in 10 women can be affected by it. It can develop at any age, but it is more common in people aged over 40 years or in those who have previously injured a joint.
Risk Factors And Causes
Osteoarthritis does not have a specific, single cause. However, there are certain risk factors which put you at risk of having this condition in some joints. These include:
- Family history of osteoarthritis – genetics play a role
- Being overweight (knees and hips at greater risk)
- Past history of injury to the joint, such as a dislocation or a fracture (knees, hips, hands)
- Increasing age
- Frequent climbing, squatting and kneeling (knees)
- Heavy weight lifting jobs (hips)
- Repetitive use of the hands
Symptoms
Symptoms can vary from person to person and change within the same person over time. Some of the common symptoms include:
- Joint stiffness and pain associated with movement
- Joint swelling and instability
- Muscle weakness
- Reduced range of movement
- Sounds within the joints
How Is It Diagnosed?
If you are experiencing joint pains, it is important to see your doctor for a diagnosis and management plan. Many different conditions can cause joint pains and they require different treatments.
Plain x-rays are sometimes used to confirm the diagnosis of osteoarthritis or to assist with planning interventions, such as surgery. A magnetic resonance imaging (MRI) is rarely required.
How Is Osteoarthritis Managed?
There is no cure for osteoarthritis, but most people with osteoarthritis can manage their symptoms well and continue with daily activities, while living a healthy and enjoyable life. Be careful of any products or treatments that claim to cure osteoarthritis completely – ask your doctor.
Healthy Diet
Extra body weight increases stress on many joints, especially the knees, hips and lower back. If you are overweight, losing weight can help decrease pain and limit further damage to your joints. While there is no diet that will cure osteoarthritis, a healthy diet can definitely help.
Limit your intake of harmful dietary fats that are found in red meat, poultry and full-fat dairy products. Too much of these increases unhealthy cholesterol (LDL), which is linked to increase cartilage damage in people with osteoarthritis. Instead, opt for healthier fats found in vegetable oils, avocados, nuts and seeds, fish and fish oil supplements.
Regular Exercise
Regular exercise is one of the most effective treatments for managing osteoarthritis. Choose activities that you enjoy & are convenient for you to do. Consulting a Physiotherapist can help. The exercise mix which helps improve symptoms of Osteoarthritis include:
- Flexibility — exercises like Yoga and muscle stretches can help maintain or improve your joint and muscle movements
- Muscle strengthening — exercises with weights & resistance bands improve muscle strength, which takes pressure off sore joints, strengthens bones and improves balance
- Fitness — Brisk walking and cycling improve the health of your heart and lungs
Special Footwear And Devices
Taping the joint, wearing braces, or using shoe insoles (Orthoses) that improve your body alignment when standing and walking can help. Your physiotherapist can guide you.
Pain Management
Ask your doctor about the best pain relief to use for your type of osteoarthritis since some medicines are only effective for certain joints,are not supported by clinical evidence, or have the risk of serious side effects. Paracetamol and non-steroidal anti-inflammatory drugs (NSAIDs) can help. NSAIDs also come in the form of gel and creams and can be used for some joints like the knee. NSAIDs tablets can cause stomach ulcers and bleeding if used long term without a doctor’s advice, which is why it’s so important to heed their advice.
Sometimes corticosteroid injections (a type of steroid) are used to reduce inflammation within the joints. These don’t last long-term and can damage the joint if you inject them more than once every 4 months.
Surgery
In most cases of osteoarthritis, surgery is not required. However, if you have tried all non-surgical treatments options without success and you are still experiencing significant pain and loss of function, then surgery may be an option.
The most common surgery for osteoarthritis is a total joint replacement. When considering surgery you should be informed about what it involves, the rehabilitation process, it’s likely benefits and any potential risks.








What do you think?
You must be logged in to post a comment.